Untreated Hyperemesis Can Lead to Preterm Birth. What Is the Cause of the Preterm Birth?
Review Article Volume 1 Result ii
Hyperemesis gravidarum-a serious outcome during pregnancy: in-depth clinical review and treatment modalities
Obrowski Michael,1 Obrowski Stephanie2
1Primary Physician and Surgeon of Wilderness Physicians, Europe
2Medical University of Lodz, President of Wilderness Physicians, Europe
Correspondence: Michael Obrowski, MD, Assistant Professor of Anatomy, 43C Zeligowskiego Street, #45, Lodz, Poland ninety-644, Europe
Received: November 23, 2022 | Published: Dec 4, 2015
Citation: Obrowski One thousand, Obrowski S. Hyperemesis gravidarum–a serious issue during pregnancy: in-depth clinical review and treatment modalities. MOJ Womens Health. 2015;1(2):38-47. DOI: 10.15406/mojwh.2015.01.00010
Download PDF
Abstruse
Hyperemesis gravidarumi is the medical condition of extreme, persistent nausea and vomiting during pregnancy. It is a serious complication of pregnancy that is characterized by intractable nausea, airsickness and dehydration. Information technology is estimated to affect 0.5–2.0% of significant women.ii–iv Malnutrition and other serious complications, such as fluid or electrolyte imbalances may also result from this event. This serious condition, if left unchecked, tin lead to dehydration, weight loss, and electrolyte imbalances. Hyperemesis gravidarum differs from Forenoon Sickness.5 Morning sickness is characterized by nausea, with or without vomiting. Morning sickness is most mutual during the first trimester, sometimes beginning as early as ii weeks afterwards conception and affects upwards to 90% of women.6 Oft, morning sickness is the starting time indication to a woman that she is pregnant. The cause of this nausea and vomiting during pregnancy, which usually subsides afterwards the starting time trimester, is believed to be related to the rapidly ascension blood level of a hormone called Human being Chorionic Gonadotropin (HCG). HCG is released by the placenta.
Keywords: hyperemesis gravidarum, forenoon sickness, human chorionic gonadotropin (HCG), β-man chorionic gonadotropin (β-hCG), phocomelia, thalidomide, low, anemia, hyponatremia, wernicke's encephalopathy, kidney failure, fundamental pontine myelinolysis, coagulopathy, atrophy, mallory-weiss tears, hypoglycemia, jaundice, malnutrition, pneumomediastinum, rhabdomyolysis, deconditioning, DVT (deep vein thrombosis), pulmonary embolism, splenic avulsion, vasospasms of cerebral arteries, fetal growth retardation, hyperolfaction, ptyalism (hypersalivation)
Abbreviations
HCG, human chorionic gonadotropin; Β-hCG, Β-human chorionic gonadotropin; DVT, deep vein thrombosis; TMP-SMX, trimethoprim and sulfamethoxazole; EBV, epstein barr virus; ALT, alanine aminotransferase; AST, aspartate aminotransferase; ALP, alkali metal phosphatase, PT, prothrombin time; CBC, consummate blood cell; AFLP, astute fatty liver of pregnancy; DKA, diabetic ketoacidosis; GTD, gestational trophoblastic illness; BUN, blood urea nitrogen; NS, normal saline; OT, over-the-counter
Causes of hyperemesis gravidarum
In that location are numerous theories regarding the cause of Hyperemesis gravidarum, simply the crusade(south) remains controversial. It is thought that Hyperemesis gravidarum is due to a combination of factors which may vary betwixt women and include: genetics,two obesity (a major gene), body chemistry and overall health.vii I other factor is an adverse reaction to the hormonal changes of pregnancy, in particular, elevated levels of β-Human Chorionic Gonadotropin (β-hCG).8,ix This theory would also explain why Hyperemesis gravidarum is about frequently encountered in the first trimester (often around 8–12 weeks of gestation), as hCG levels are highest at that time and decline subsequently. Another postulated cause of Hyperemesis gravidarum is an increment in the maternal levels of estrogens (which can have the effect of decreasing intestinal motility and gastric emptying fourth dimension leading to nausea and/or airsickness).one Withal, Hyperemesis gravidarum is considered a rare complexity of pregnancy. Dissimilar morning sickness, Hyperemesis gravidarum can cause severe weight loss from x% upwards to forty% of one's pre-pregnancy weight. Information technology tin can also be life-threatening if not treated due to astringent electrolyte imbalances that occur from severe, continuous vomiting. Also, unlike forenoon sickness, Hyperemesis gravidarum tin can last throughout the pregnancy and usually comes with constant vomiting, merely e'er with constant nausea. A modest percentage of patients with Hyperemesis gravidarum rarely vomit, but the nausea still causes about (if not all) of the same bug that Hyperemesis gravidarum with vomiting does.
Signs and symptoms
When Hyperemesis gravidarum is severe or inadequately treated, regardless of the reason, it may upshot in the following symptoms:
- Loss of 10 to 40% or more of pre-pregnancy trunk weight
- Dehydration, causing ketosisten and constipation
- Nutritional disorders such as Vitamin B1 (Thiamine) deficiency, Vitamin B6 (Pyridoxine) deficiency or Vitamin B12 (Cobalamin) deficiency
- Metabolic imbalances such equally metabolic ketoacidosisten or thyrotoxicosis11
- Physical and emotional stress of pregnancy on the body
- Difficulty with activities of daily living
- Symptoms can be aggravated by hunger, fatigue, prenatal vitamins (specially those containing iron) and nutrition.12
- Many sufferers of Hyperemesis gravidarum are extremely sensitive to odors in their environment; sure smells may exacerbate symptoms which is known equally Hyperolfaction. Ptyalism or hypersalivation, is another symptom experienced by some women suffering from Hyperemesis gravidarum.
- Hyperemesis gravidarum tends to occur in the first trimester of pregnancyand lasts significantly longer than morn sickness. While about women volition experience almost-complete relief of morning sickness symptoms most the beginning of their second trimester. Some sufferers of Hyperemesis gravidarum will experience severe symptoms until they requite nascence to theirbaby, and sometimes even later on giving birth.13
- Unfortunately, many women that accept experienced Hyperemesis gravidarum during whatever pregnancy are at a college take chances of experiencing it withsubsequent pregnancies.
Pathophysiology
Although the pathophysiology of Hyperemesis gravidarum is poorly understood, the virtually commonly accepted theory suggests that levels of hCG are associated with it.xiv Leptin may also play a office according to recent (2006) joint inquiry written report out of Australia and New Zealand.15 Possible pathophysiological processes involved are summarized in the following Figure one.
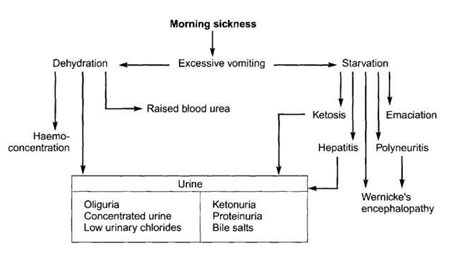
Figure 1 Pathophysiological processes.
Diagnosis
Hyperemesis gravidarum is a diagnosis of exclusion.1 Hyperemesis gravidarum canbe associated with serious maternal and fetal morbidity, such as Wernicke's encephalopathy, coagulopathy, peripheral neuropathy,4 fetal growth retardation, and even maternal and fetal decease. Women experiencing Hyperemesis gravidarum are often dehydrated and lose weight despite efforts to consume.16,17 The onset of the nausea and airsickness in Hyperemesis gravidarum is typically before the twenty-second calendar week of pregnancy.1
Differential diagnosis
The post-obit is a simple listing of all of the possible differential diagnoses that need to exist kept in the back of the clinician's mind. This list is by no ways all inclusive, information technology is based on the primary author'south personal experience in Obstetrics and Gynecology. Although Hyperemesis gravidarum is usually easily established by taking a thorough history and physical test, do non miss any of the following possible differentials:
Infections (usually accompanied past fever or associated symptoms)
Urinary Tract Infection
- Common in females, more mutual during pregnancy due to voiding issues
- Easily diagnosed in the office with Urine Dipstick
- Confirm with sterile, midstream urine sample
- Exercise not delay treatment as infection can travel to kidneys
- Infection can exist in whatever part of the urinary system
- Kidneys, Ureters, Bladder, Urethra.
- Most infections involve the float and the urethra.
- Care for carefully, cull antibiotics based on safety to female parent and fetus
Antibiotics more often than not considered prophylactic during pregnancy:
- Amoxicillin
- Ampicillin
- Clindamycin
- Erythromycin
- Penicillin
- Nitrofurantoin
- Do not use Tetracycline (including Doxycycline and Minocycline) under whatever circumstances
- Tetracycline can impairment a pregnant woman's liver
- Tetracycline can as well permanently discolor a babe'south teeth.
- Two antibiotics commonly used together to treat urinary tract infections, Trimethoprim and Sulfamethoxazole (TMP-SMX, also normally sold every bit Bactrim) may be linked with an increased take a chance of birth defects – use with caution.
- This is a common listing of antibiotics used for UTI's – the authors have no responsibility for their use –delight use your clinical judgement and experience.
Hepatitis
- Acute viral hepatitis is the most common cause of jaundice in pregnancy. The clinical course of most viral infections is non affected by pregnancy. Jaundice is a characteristic feature of liver disease. Clinical signs and symptoms are duplicate between the diverse forms of viral hepatitis. The differential diagnosis requires serologic testing for a virus-specific diagnosis. Diagnosis is by biochemical assessment of liver function.
- The differential diagnosis should include other forms of viral hepatitis
- Mononucleosis and Epstein-Barr Virus (EBV)
- Autoimmune Disease
- Widespread Systemic Infection with Liver Failure
- Patients presenting with jaundice during pregnancy often require a workup to differentiate obstructive gall float or bile duct disease, severe preeclampsia, HELLP Syndrome (hemolysis, elevated liver enzyme levels, depression platelet count), or acute fatty liver of pregnancy from viral hepatitis.
- The nigh useful tests to diagnose hepatitis include laboratory evaluation of urine bilirubin and urobilinogen, total and direct serum bilirubin, alanine aminotransferase (ALT) and/or aspartate aminotransferase (AST), alkaline phosphatase (ALP), prothrombin time (PT), total protein, albumin, consummate blood cell (CBC) count and in severe cases, serum ammonia.
Bacterial meningitis
- Bacterial meningitis is usually severe. Most people with meningitis recover however it can cause serious complications, such as encephalon damage, hearing loss, or learning disabilities.
- Meningitis infection may show upward in a person by a sudden onset of fever, headache, and stiff neck. The patient may exhibit other symptoms, such as:
- Nausea
- Vomiting
- Photophobia (Increased sensitivity to lite)
- Altered mental condition
- Babies younger than 1 month old are at a college risk for severe infections such every bit meningitis.
- In newborns and infants, the classic meningitis symptoms of fever, headache and neck stiffness may be absent or hard to notice.
- The babe may appear to be tiresome or inactive (lack of alertness), irritable, airsickness or feeding poorly. The babe may exhibit a bulging fontanelle or abnormal reflexes, which can also be signs of meningitis.
- There are several pathogens that tin can cause bacterial meningitis.
- Leading causes of bacterial meningitis include:
- Haemophilus influenzae(most often Type B, HiB)
- Streptococcus pneumoniae
- Grouping B Streptococcus
- Pregnant women who test positive for Group B Streptococcus tin pass the leaner to their baby, virtually often during labor and vaginal nascence. A newborn infected with Grouping B Strep bacteria can develop meningitis or other life-threatening infections soon after birth.
- Listeria monocytogenes
- Neisseria meningitidis
- If meningitis is suspected, samples of blood or cerebrospinal fluid are collected and sent to the laboratory for testing.
- Practice not delay handling – use caution in the pregnant patient regarding which drugs are used to treat Bacterial Meningitis
- Bacterial Meningitis can cause spontaneous abortion of the fetus
Gastrointestinal disorders(usually accompanied by abdominal hurting)
Gastroenteritis
- Many unlike causes of gastroenteritis exist, including viruses or bacteria.
- Gastroenteritis usually lasts simply a couple of days, whether the patient is pregnant or not.
- Dehydration can crusade premature contractions, fatigue and dizziness.
- Advise your patient to drinkable plenty of fluids including water, soda, tea, chicken soup or whatever she can take in without vomiting.
- Symptoms that are very severe or persist for more than 2 or 3 days may require 4 Rehydration.
Appendicitis
- Acute appendicitis is the about common general surgical problem encountered during pregnancy. The diagnosis is challenging during pregnancy because of the relatively high prevalence of abdominal/gastrointestinal discomfort, anatomic changes related to the enlarged uterus and physiologic leukocytosis of pregnancy.
- Appendiceal rupture occurs more frequently in pregnant women, particularly in the third trimester, perchance because of the reluctance to operate on significant women delays diagnosis and treatment
- Patient Presentation: In the "classic" presentation of appendicitis, the patient describes the onset of abdominal pain as the first symptom.
- The hurting is periumbilical initially and then migrates to the right lower quadrant as the inflammatory process progresses.
- Anorexia, nausea and vomiting, if present, follow the onset of pain.
- Fever upward to 101.0ºF (38.3ºC) and leukocytosis develop later.
- Many pregnant patients have a nonclassical presentation, especially in late pregnancy, with symptoms such as heartburn, bowel irregularity, flatulence, malaise, or diarrhea.
- If the appendix is retrocecal, patients often complain of a dull ache in the right lower quadrant rather than localized tenderness.
- Rectal or vaginal examination in such patients is more than likely to elicit pain than abdominal examination.
- A pelvic appendix can cause tenderness below McBurney'south Point; these patients often mutter of urinary frequency and dysuria or rectal symptoms, such as tenesmus and diarrhea.
- The most common symptom of appendicitis, i.due east., right lower quadrant pain, occurs close to McBurney's point in the majority of significant women, regardless of the stage of pregnancy; however, the location of the appendix migrates a few centimeters cephalad with the enlarging uterus, so in the third trimester, pain may localize to the mid or even the upper right side of the abdomen.
- Surgery for appendicitis must be adamant on a run a risk-to-benefit ratio. Consultation with a Full general Surgeon and Anesthesiologist is vital to ascertain the risk to the fetus from anesthesia compared to the gamble of a ruptured appendix and subsequent peritonitis, which can kill both the mother and fetus.
Cholecystitis
- Acute cholecystitis can be especially hard to recognize in pregnancy.
- Once diagnosed, the initial direction plan should exist bourgeois and include antibiotic therapy.
- Subsequent management depends on the gestational age at diagnosis.
- Surgical therapy, when indicated, should not be delayed and a planned intervention during the 2nd trimester appears to offer a ameliorate outcome than surgery performed nether emergent conditions.
Cholestasis of pregnancy
- Cholestasis of pregnancy occurs in late pregnancy and triggers intense itching, normally on the hands and feet merely oft on many other parts of the torso.
- Cholestasis of pregnancy can brand you lot intensely uncomfortable but poses no long-term chance to an expectant mother.
- For the developing baby, however, cholestasis of pregnancy can be dangerous. Early delivery is recommended.
- The term "cholestasis" refers to any condition that impairs the catamenia of bile from the liver. Pregnancy is one of many possible causes of cholestasis. Other names for cholestasis of pregnancy include obstetric cholestasis and intrahepatic cholestasis of pregnancy.
Pancreatitis
- About cases of acute pancreatitis in pregnancy are caused by gallstone disease. It is thought with the weight and hormonal changes induced past pregnancy, gallstones are more than likely to form and thus travel down the common bile duct to obstruct the pancreas duct outflow.
- Another proposed machinery for acute pancreatitis in pregnancy is loftier triglyceride levels.
- Hormonal changes of pregnancy can predispose sure women to developing this status. When the triglyceride levels go too high, oxygen cannot adequately travel to the pancreas via the bloodstream, and pancreatitis can ensue.
- All of the other reasons for developing acute pancreatitis such equally alcohol corruption, reaction to certain medications, trauma to the pancreatic duct can likewise pb to acute pancreatitis in pregnancy
- Treatment of acute pancreatitis in pregnancy is similar to that of non-pregnant patients with some exceptions. Resting the digestive tract by not eating, pain command and aggressive fluids given through an IV line are essential.
- If the reason is gallstone pancreatitis, removal of the gallbladder is deferred until later pregnancy. Oft, a stent can be placed into the bile duct to temporize the situation until operative resection is needed.
- If waiting until the end of pregnancy is non possible, surgical resection can more often than not be performed safely.
- If the cause of acute pancreatitis is due to elevated triglycerides, certain medications and dietary modifications can be used to help prevent recurrent attacks.
- If the attack occurs late in the 3rd trimester, delivery is usually advocated, as this volition crusade an immediate decrease in the triglyceride levels.
- Other causes of acute pancreatitis, such equally traumatic ductal injury, demand to be carefully assessed on an individual basis.
Astute fat liver of pregnancy (AFLP)
- Astute fatty liver of pregnancy is a serious complexity unique to pregnancy get-go described past Sheehan in 1940. It is characterized past micro vesicular steatosis in the liver. The foremost cause of AFLP is idea to be due to a mitochondrial dysfunction in the oxidation of fatty acids leading to an accumulation in hepatocytes. The infiltration of fatty acids causes acute liver insufficiency, which leads to most of the symptoms that present in this status. If not diagnosed and treated promptly, AFLP tin outcome in high maternal and neonatal morbidity and mortality.
- AFLP is unique to pregnancy. There does not appear to be a predilection for whatsoever geographical area or race. It appears to occur more commonly in primiparous women than multiparous women
- Due to advances in diagnostic strategies and supportive care, maternal mortality and perinatal morbidity of AFLP has declined. In the 1980s, Kaplan reported a bloodshed rate for both mother and fetus of nearly 85%. Maternal mortality is now estimated to be 12.5-18%, with a neonatal mortality charge per unit of 7-66%.
- While laboratory abnormalities may persist after delivery, in rare cases patients may progress to hepatic failure with the need for liver transplantation.
- Morbidity of the infant includes increased take a chance of cardiomyopathy, neuropathy, myopathy, non-ketotic hypoglycemia, hepatic failure and death associated with fat acrid oxidation defects in newborns.
- Delivery of the fetus, regardless of gestational age, is the only treatment for acute fatty liver of pregnancy (AFLP) once the diagnosis has been made.
- Mode of delivery is dependent on the following several factors:
Fetal status: Many fetuses demonstrate evidence of asphyxia and hypoxia; therefore, close monitoring of fetal status is necessary, along with the ability to expedite delivery should fetal compromise be evident.
Maternal coagulation status: Due to coagulation abnormalities that tin can accompany AFLP, patients may need to have replacement of their coagulation factors should cesarean delivery be necessary.
Likelihood of success with induction of labor: If delivery cannot be safely accomplished inside 24 hours from the time of diagnosis, so a Caesarean Section is mandatory.
Direction of severe hypoglycemia: Necessary to avoid coma and death. Patients require at least a 5% Dextrose solution to maintain claret glucose levels. Blood glucose should be monitored closely until hepatic function returns and the patient tolerates a regular diet.
Renal function: can also be affected by several factors, including maternal hemorrhage, which tin atomic number 82 to astute tubular necrosis and hepatorenal syndrome. Fluid residuum should be closely monitored, as patients may develop pulmonary edema due to low plasma oncotic pressures
Peptic ulcer
- Peptic ulcer disease developing during pregnancy is relatively rare. Certainly, gastroesophageal reflux symptomatology and Hyperemesis gravidarum are the primary pregnancy-associated upper gastrointestinaltract illnesses. The symptoms of dyspepsia accompanies all three diagnoses and makes information technology difficult to determine whether peptic ulcer is playing a function in the patient's symptomatology.
- Patients with a previous history of complicated peptic ulcer diatheses should exist suspected of having recurrent ulcer illness and treated accordingly. Endoscopy is not to be feared if needed to confirm a diagnosis of peptic ulcer disease or to aid in the diagnosis of the patient with upper alimentary canal hemorrhage.
- At that place is thought to exist some improvement in peptic ulcer affliction with pregnancy, which may be secondary to lower gastric acid output and increased protective fungus production associated with elevated progesterone levels.
- This may afford some level of protection against this disease process in pregnant women.
- Patients who are smokers and take a previous history of peptic ulcer disease are at highest risk for ulcer disease during pregnancy.
- Multiple agents take been found to be relatively safe and effective for ulcer healing, with H2 Antagonists the mainstay of therapy during pregnancy.
Small bowel obstacle
- The most mutual cause of bowel obstacle in pregnancy is adhesions secondary to prior surgery or disease (Effigy 2). In one study, 77% of the 66 cases presented with known obstruction due to adhesions from previous abdominal surgery, pelvic surgery, or pelvic inflammatory conditions.
- A previous caesarean birth can exist a contributing factor. Bowel obstruction may occur during the fourth to fifth months of pregnancy when the uterus rises into the abdomen only virtually often occurs in the third trimester or postpartum.
- When an obstruction occurs, there is significant risk for severe morbidity or mortality for both female parent and fetus, handling needs to occur as soon as possible.
- Delays due to errors in diagnosis, delayed diagnosis, or reluctance to operate during pregnancy all add to increased risk.
- The maternal mortality rate in ane written report was 4 deaths in 66 women diagnosed with obstruction (Effigy ii).
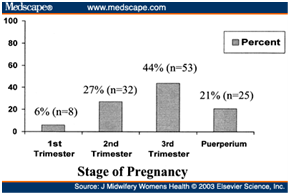
Figure 2 Stage of Pregnancy.
Metabolic
Thyrotoxicosis (Hyperthyroidism) 14
Graves-basedow affliction: named subsequently the Irish Doctor (Robert Graves) and the High german Md (Karl von Basedow) who described several cases in 1835 and 1840. Information technology was actually first described past Parry a few years earlier. In Europe the disease is known every bit Basedows' Disease. In all countries it is as well known as "Thyrotoxicosis". The affliction has a genetic component, although not every fellow member of the afflicted families will suffer this condition. It is more common in females than in males.
Thyroid stimulating antibody: Graves' affliction is an autoimmune disorder. It is caused by an abnormal protein called the thyroid stimulating antibody. This antibody stimulates the thyroid gland to produce large amounts of thyroid hormone in an uncontrolled manner. In normal people, the production of the thyroid stimulating antibody (and other aberrant antibodies) is prevented by a surveillance system. This arrangement consists of certain blood cells called suppressor and helper lymphocytes, Killer Cells and other constituents. Measurement of the thyroid stimulating antibody nowadays in the claret of patients with Graves' illness is non unremarkably necessary, in social club to institute the diagnosis.
Clinical Features: The signs and symptoms of Graves' hyperthyroidism are due to the effects of excess amounts of thyroid hormone on torso role and metabolism. Common symptoms include weight loss, nervousness, irritability, intolerance to hot conditions, excessive sweating, shakiness, and muscle weakness. Other signs include a rapid pulse, loss of trunk fat, loss of muscle bulk, thyroid enlargement (goiter), fine tremors of the fingers and hot, moist, velvety skin.18 Clinically evident eye signs (ophthalmopathy) occur in patients with Graves' disease. Fortunately only approximately 5% are severe. The optics, which burl from their sockets can be ruby-red and watery and the lids are swollen. Often the eyes do non move normally because the bloated heart muscles are unable to work precisely and patients can experience double vision. Some patients with Graves' hyperthyroidism may have slightly bulging eyes because of spasm of the musculus of the lids, giving them a staring appearance.
Thyroid hormones: have a broad multifariousness of effects on the body and the signs and symptoms reverberate these.
All the metabolic processes are "speeded upwardly". Pulse rate is rapid (over 100 bpm) and occasionally irregular (atrial fibrillation) Bowel function is increased (diarrhea) Sweat glands piece of work excessively, causing the patient to often complain of hyperhidrosis. The nervous system is also stimulated so that the patient becomes irritable and nervous. Despite an increment in ambition, the patient normally loses weight because food intake cannot keep upward with the increased breakup of body proteins. The cease effect is a thin, hot, nervous patient with bulging eyes and goiter - a classical clinical situation apace recognized by any medical practitioner who has previously seen such a patient.
Treatment: Graves' hyperthyroidism is caused by a genetically determined abnormality of the immune system, therefore the trouble is complex and at that place is at present no specific treatment for the underlying aberration. Since the end result of this problem is an over stimulation of thyroid function, treatment of the symptoms requires blocking thyroid hormone product with antithyroid drugs, destroying the thyroid cells with radioactive iodine or surgically removing the thyroid gland (thyroidectomy).
Radioactive iodine: Although radioactive iodine is by far the simplest and near convenient treatment, its use in younger adults and children has previously been a matter of business because of the possible harmful effects of radiation. Radioactive iodine has been used for over 40years and in that location is no known evidence of any harmful effects. In North America most thyroid specialists would recommend its apply in most patients with Graves' disease over the age of 20-25 considering it has a higher chance of long-term success (resolution of hyperthyroidism) than antithyroid drugs. Its use in adolescents is increasing. However, it occasionally aggravates the eye sight and preventive handling with corticosteroids is sometimes warranted. Radioactive iodine is unremarkably given in the form of a capsule. The dose is calculated from the size of the goiter and the 24hour iodine uptake obtained by performing a "Thyroid Uptake Examination." Considering radioactive iodine takes several weeks to accept its full upshot, antithyroid tablets are sometimes given until such time as the full issue occurs.
Antithyroid drugs: Antithyroid drugs (such as Propylthiouracil and Methimazole) are ordinarily used in children and adults under the age of 20-25. It may also be used at whatsoever historic period so equally to bring nigh remissions, or prior to ablation therapy. In that location are 2 main drawbacks with this type of treatment: Patients must have tablets for many months or years, the recommended menses of fourth dimension for the handling is 12 to 18 months;Once treatment is stopped, in that location is merely about a l% gamble that the disease will not flare upward once more. Therefore almost patients require additional treatments. In addition, a very small percentage suffer side furnishings that very rarely can be astringent (liver problems, low white blood cell count). Because of the recent testify of side effects of Propylthiouracil on liver office, specially in children, the FDA has issued a warning for its utilise. Propylthiouracil is nevertheless the treatment of choice during pregnancy since in that location is unclear evidence about Methimazole side effects in the fetus (aplasia cutis, choanal atresia). It is preferable to treat the hyperthyroidism before because pregnancy. Another medication that can be given to treat the symptoms of hyperthyroidism is Propranolol or other beta-blockers. This drug blocks the effects of excess thyroid hormones on the middle, blood vessels, and nervous system, but has no direct effect on the thyroid gland. It is contraindicated in patients with asthma.
Addison'southward affliction
Women with diagnosed and undiagnosed autoimmune Addison's disease are at increased adventure for preterm birth, low nativity weight and other unfavorable pregnancy outcomes, according to results of a Swedish population-based cohort study.19 In addition, women with autoimmune Addison'due south illness had a reduced parity compared with other women. Risks for congenital malformations or infant death were not associated with diagnosed or undiagnosed autoimmune Addison's affliction.
Diabetic ketoacidosis (DKA) xx
The occurrence of diabetic ketoacidosis in pregnancy compromises both the fetus and the mother. It usually occurs in the later stages of pregnancy and is too seen in newly presenting Type 1 Diabetic Patients. Despite improvement in its incidence rates and outcomes over the years, information technology yet remains a major clinical problem since it tends to occur at lower blood glucose levels and more chop-chop than in non-pregnant patients often causing delay in the diagnosis. Diabetic ketoacidosis (DKA) is an acute medical emergency associated with fetal loss rates in excess of fifty%. Maternal mortality rates are generally less than 1%. DKA in pregnancy about usually occurs in women with pregestational, insulin dependent diabetes who are poorly controlled or in women newly diagnosed with insulin dependent diabetes. DKA may be provoked by an exposure to a stress such as infection, surgery, or labor.
Hyperparathyroidism
- Hyperparathyroidism (parathyroid disease with high calcium) occurring during pregnancy is a very serious problem. Hyperparathyroidism during pregnancy puts both the mother's and kid'due south life at risk, and the run a risk for life-long calcium problems for the child exists. Hyperparathyroidism during pregnancy is treated with mom's surgery during the late first or early 2d trimester.
- Hyperparathyroidism during pregnancy is very rare. However, this can exist a very serious trouble for both mother and kid. It must be addressed in the correct fashion for the best results and the obstetrician and the surgeon must communicate then that both the mother and the child practise well.
Potential Risks of Hyperparathyroidism During Pregnancy:
- Increased risk of hypertension (pre-eclampsia and eclampsia) in the mother (about xx times more than common).
- Risk of miscarriage can be as high every bit 85 percent.
- Risk of permanent hypoparathyroidism in baby (failure of the parathyroid glands to form).
- Risk of centre rhythm bug during labor/delivery.
- Risk of premature birth.
- Take chances of seizures in the baby during outset few days of life (due to LOW levels of calcium).
- This is one of the true emergencies with hyperparathyroidism. Do non fool around here! Bring in a neonatologist if possible to assist you with the infant.
Other drugs
Antibiotics: Antibiotics were discussed earlier in this report. The main reason to mention information technology here again briefly, is to NEVER give unnecessary antibiotics and to carefully choose which one is being prescribed if an antibiotic is absolutely necessary.
Iron supplements
When a adult female is pregnant, she will demand about twice the amount of fe as she normally did before condign pregnant. The body uses iron to brand extra blood for your baby. Unfortunately, near 50% of meaning women do not get enough of this important mineral. Eating iron-rich foods and taking extra iron (approximately xxx mg. per day) will be sufficient. The human body uses fe during pregnancy to make extra hemoglobin for the mother and the fetus. Iron also helps motility oxygen from the mother'due south lungs to the rest of the mother's and fetus'due south torso. Getting plenty fe can forestall a condition of likewise few cerise blood cells that can make y'all feel tired, called iron deficiency anemia. Having anemia tin cause your baby to exist born likewise small or as well early.
Prenatal Vitamins
Propose your patient to eat a healthy nutrition during pregnancy, which tin lessen the effects of morn sickness and Hyperemesis gravidarum. Prescribe your patient with a expert Prenatal Vitamin, numerous ones are available depending on where yous alive. Prescription Prenatal Vitamins are preferred in lieu of OTC Vitamins equally the prescription vitamins are specifically formulated for significant patients.
A good, well-formulated Prenatal Vitamin will contain at least the following:
- 400micrograms (mcg) of folic acid.
- 400IU of vitamin D.
- 200 to 300milligrams (mg) of calcium.
- 70mg of vitamin C.
- 3mg of thiamine.
- 2mg of riboflavin.
- 20mg of niacin.
- 6 mcg of vitamin B12.
- 10mg of vitamin Eastward
- 15mg of zinc
- 17mg of atomic number 26
- 150mcg of iodine
Prenatal vitamins contain many vitamins and minerals. All of them comprise folic acid, fe, iodine, and calcium which are especially of import during pregnancy. Folic acid helps foreclose neural tube birth defects, which affect the brain and spinal string.
Gestational trophoblastic diseases (rule out with urine β-hCG)
Molar pregnancy
- A Tooth Pregnancy is an abnormal form of pregnancy in which a non-viable fertilized egg implants in the uterus and volition neglect to come up to term. A molar pregnancy is a gestational trophoblastic disease which grows into a mass in the uterus that has bloated chorionic villi. These villi grow in clusters that resemble grapes. Even though information technology isn't an embryo, this growth triggers symptoms of pregnancy.
- A tooth pregnancy should be treated right away. This volition make sure that all of the tissue is removed. This tissue can cause serious problems in some women.
- About 1 out of 1,500 women with early pregnancy symptoms has a molar pregnancy.
- Molar pregnancy is thought to be caused past a trouble with the genetic information of an egg or sperm. In that location are two types of molar pregnancy - complete and partial.
Complete molar pregnancy: An egg with no genetic data is fertilized by a sperm. Information technology does not develop into a fetus but continues to abound as a lump of abnormal tissue that looks a bit like a cluster of grapes and can fill the uterus.
Partial tooth pregnancy: An egg is fertilized by two sperm. The placenta becomes the tooth growth. Any fetal tissue that forms is probable to accept severe defects. A Molar Pregnancy causes the same early symptoms that a normal pregnancy does, such as a missed menstruum or morning sickness. But a molar pregnancy usually causes other symptoms too, which may include:
- Bleeding from the vagina.
- A uterus that is larger than normal.
- Severe nausea and vomiting.
- Signs of hyperthyroidism. These include feeling nervous or tired, having a fast or irregular heartbeat, and sweating a lot.
- An uncomfortable feeling in the pelvis.
- Vaginal discharge of tissue that is shaped similar grapes. This is usually a sign of a "miscarriage" of a molar pregnancy.
- Almost of these symptoms tin besides occur with a normal pregnancy, a multiple pregnancy, or a miscarriage.
Choriocarcinoma
A cancerous, trophoblastic cancer, usually of the placenta. It is characterized past early hematogenous spread to the lungs. It belongs to the cancerous cease of the spectrum in gestational trophoblastic disease (GTD). Information technology is also classified as a germ cell tumor and may ascend in the testis or ovary.
Choriocarcinoma of the placenta during pregnancy is preceded by:
- Hydatidiform Mole (50% of cases)
- Spontaneous Abortion (20% of cases)
- Ectopic Pregnancy (2% of cases)
- Normal Term Pregnancy (20-thirty% of cases)
- Hyperemesis gravidarum
- Rarely, choriocarcinoma occurs in primary locations other than the placenta. Very rarely, it occurs in the testicles and elements of choriocarcinoma in a mixed testicular tumor have no prognostic importance.
- Although trophoblastic components are mutual components of mixed germ cell tumors, pure choriocarcinoma of the adult testis is rare.
- Pure choriocarcinoma of the testis represents the most aggressive pathologic variant of germ cell tumors in adults, characteristically with early on hematogenous and lymphatic metastatic spread.
- Considering of early spread and inherent resistance to anticancer drugs, patients have poor prognosis.
- Choriocarcinomas can likewise occur in the ovaries with an equally poor prognosis.
Clinical investigations
Common investigations include blood urea nitrogen (BUN) and electrolytes, liver part tests, urinalysis and thyroid function tests. Hematological investigations include hematocrit levels, which are usually raised in Hyperemesis gravidarum. An ultrasound scan may exist needed to know gestational condition and to exclude tooth or partial molar pregnancy.
Management of hyperemesis gravidarum patient
Dry bland food and oral rehydration are first-line treatments. Due to the potential for severe dehydration and other complications, Hyperemesis gravidarum is treated as an emergency. If conservative dietary measures fail, more than extensive treatment suchs as the use of antiemetic medications and intravenous rehydration may be required. If oral nutrition is insufficient, intravenous nutritional support may exist needed. For women who require hospital access, thromboembolic stockings or low-molecular-weight heparin may also be used every bit measures to prevent the formation of a blood clot.
Intravenous fluids
IV hydration often includes supplementation of electrolytes as persistent vomiting frequently leads to not only a fluid deficiency, which can cause a patient to get into daze with a dropping blood pressure level and an increased pulse rate but also severe electrolyte and vitamin deficiency. Unfortunately, most patients do not seek treatment in the hospital or office until they are in trouble – so activity must exist taken apace. Supplementation for lost thiamine (Vitamin B1) must be considered to reduce the run a risk of Wernicke'southward Encephalopathy, Vitamins A and B are depleted inside two weeks and so extended malnutrition indicates a need for evaluation and supplementation. In addition, electrolyte levels should be monitored and supplemented; of particular business are sodium and potassium.
Some patients do good from what is colloquially chosen a "Banana Bag", often used in malnourished alcoholics. The vitamins and supplements are sometimes available in v to 10 cc. ampules which are added to a liter of whatever fluid the physician chooses for rehydrating the Hyperemesis gravidarum patient. Once more, the clinical judgement and patient presentation are nearly important when utilizing whatever Iv fluids for rehydration therapy. If pre-made ampules of vitamins or pre-fabricated banana bags are not available in your hospital, the typical limerick of a banana bag is i liter of Sodium Chloride 0.9% (NS-Normal Saline) with:
- Thiamine 100 mg
- Folic acrid one mg
- MVI ane amp (Multivitamin for infusion, ane ampule)
- Magnesium sulfate 3 g
The solution is typically infused over four to 8 hours or as per physician's orders which should be based on patient status. Frequently you tin can piggyback 250 cc. of D5W or Ringer's Lactate Solution onto the banana bag infusion set. All these IV fluids deed differently but are very efficacious in helping the patient feel ameliorate. The primary writer of this report will utilize Ringer'southward Lactate Solution in identify of the Normal Saline 0.9% in making up a banana pocketbook. He has had excellent results in severe cases of Hyperemesis gravidarum.
One liter of Ringer'southward lactate solution contains:
- 130 mEq of sodium ion = 130 mmol/50
- 109 mEq of chloride ion = 109 mmol/50
- 28 mEq of lactate = 28 mmol/Fifty
- four mEq of potassium ion = four mmol/Fifty
- iii mEq of calcium ion = one.5 mmol/L
Ringer'due south Lactate has an osmolarity of 273 mOsm/Fifty. The lactate is metabolized into bicarbonate past the liver, which can help correct metabolic acidosis, which tin occur to a astringent extent in Hyperemesis gravidarum. Ringer'southward Lactate solution alkalinizes via its consumption in the citric acid cycle, the generation of a molecule of carbon dioxide which is then excreted by the lungs. They increase the strong ion deviation in solution, leading to proton consumption and an overall alkalinizing consequence. Afterwards IV rehydration is completed, patients in general should be advised to transition to frequent pocket-sized liquid or bland meals. After rehydration, treatment focuses on managing symptoms to allow normal intake of nutrient. However, cycles of hydration and dehydration can occur, making continuing care necessary. Dwelling care is available in the course of a PICC line for hydration and Total Parenteral Nutrition (TPN).21 Abode handling is frequently less expensive than long-term or repeated hospitalizations.
Medications
A number of antiemetics are effective and safe in pregnancy including: pyridoxine/doxylamine, antihistamines (such as diphenhydramine), and phenothiazines (such as promethazine).22 With respect to effectiveness, it is unknown if 1 is superior to another22 and there is fifty-fifty express show of meaning effect at all of pharmacological therapy in hyperemesis gravidarum.22
While pyridoxine/doxylamine, a combination of Vitamin B6 and Unisom/doxylamine (an Over-the-Counter {OTC} sleeping aid/antihistamine), is effective in nausea and vomiting of pregnancy,23 some have questioned its effectiveness in Hyperemesis gravidarum.24 The primary writer of this report has had great success with the pyridoxine/doxylamine combination, for both morning sickness and Hyperemesis gravidarum. He has delivered well over 500 babies and has recommended itprophylactically for his patients to buy these two OTC drugs and have them on mitt. Patients have reported by and large positive results, some even stating that at the first sign of nausea, they take the combination correct abroad, unremarkably with relief being obtained inside 30 minutes. Patients study taking ten to 25mg. of Vitamin B6 along with 5 to 25 mg. of Doxylamine. It appears that the dosing is patient dependent. The primary author of this article does not recommend any other medications due to inadequate, loftier quality research bachelor and as well high of a risk for fetal defects.
Some researchers land that Ondansetron may be benign, however, there are some concerns regarding an association with cleft palate25 and there is little high quality data.22 Metoclopramide is likewise used and relatively well tolerated. Evidence for the use of corticosteroids is weak; there is some evidence that corticosteroid use in pregnant women may slightly increment the risk of oral facial clefts in the baby and may suppress fetal adrenal action.1,24 However, hydrocortisone and prednisolone are inactivated in the placenta and may be used in the handling of hyperemesis gravidarum.1
Nutritional back up
Women non responding to 4 rehydration and medication may require nutritional back up. Patients might receive parenteral nutrition (intravenous feeding via a PICC Line - Peripherally Inserted Primal Catheter) or enteral nutrition (via a nasogastric tube or a nasojejunal tube). There is only limited evidence from trials to support the use of vitamin B6 to improve result. Hyperalimentation may be necessary in certain cases to help maintain volume requirements and allow weight gain.26 A physician might also prescribe Vitamin B1 (to prevent Wernicke's Encephalopathy) and Folic Acid supplementation.27
Medicines
There is tentative, unsubstantiated evidence that seems to be circulating on the Internet that ginger, either in raw, pickled (the type used on sushi) or lozenge (candy) form may be useful to relieve the symptoms of Hyperemesis gravidarum. However, according to current scientific studies, the efficacy of ginger is non clear.21 Safety concerns take besides been raised regarding its unpredictable anticoagulant22 backdrop which could have an adverse furnishings on the female parent or fetus. These authors do not advise the ingestion of whatever ginger or ginger-based products during pregnancy. Acupuncture, both traditional needle acupuncture and Acupressure Point P6 on the wrist (Pericardium 6 or Nei Guan Point) have been found to be totally ineffective for Hyperemesis gravidarum.28
Complications pregnant adult female
If Hyperemesis gravidarum is inadequately treated, Anemia, Hyponatremia, Wernicke'due south Encephalopathy, Kidney Failure, Key Pontine Myelinolysis, Coagulopathy, Atrophy, Mallory-Weiss Tears, Hypoglycemia, Jaundice, Malnutrition, Pneumomediastinum, Rhabdomyolysis, Deconditioning, DVT (Deep Vein Thrombosis), Pulmonary Embolism, Splenic Avulsion, or Vasospasms of Cerebral Arteries are possible serious consequences.ii Depression is a common secondary complexity of Hyperemesis Gravidarum and emotional support can be benign.27
Infant
The effects of Hyperemesis gravidarum on the fetus are mainly due to electrolyte imbalances acquired by Hyperemesis gravidarum in the mother.27 Infants of women with severe Hyperemesis gravidarum who gain less than 7 kg. (15.4 lbs.) during pregnancy tend to be of lower nascence weight, pocket-size for gestational age and born before 37 weeks gestation.5 In dissimilarity, infants of women with Hyperemesis gravidarum who have a pregnancy weight proceeds of more than than 7 kg. appear similar to infants from uncomplicated pregnancies.4 At that place is no significant departure in the neonatal death charge per unit in infants built-in to mothers with Hyperemesis gravidarum compared to infants born to mothers who exercise not have Hyperemesis gravidarum.two
Epidemiology
Severe, debilitating vomiting is a common condition in Hyperemesis gravidarum affecting virtually fifty% of pregnant women, with another 25% suffering from nausea.5 However, the incidence of Hyperemesis gravidarum is only 0.5–2.0%.2,3,4 After preterm labor, Hyperemesis gravidarum is the second nearly common reason for hospital admission during the first half of pregnancy.ane Factors such as infection with Helicobacter pylori, a ascent in thyroid hormone product, low age, depression body mass alphabetize prior to pregnancy, multiple pregnancies, molar pregnancies, and a past history of Hyperemesis gravidarum accept been associated with the development of Hyperemesis gravidarum.ane
Historical severe medication failures
Thalidomide (Immunoprin) is an immunomodulatory drug and the paradigm of the thalidomide course of drugs. It was prescribed for handling of Hyperemesis gravidarum worldwide, particularly in Europe. The United States FDA refused to approve the drug when it was released in 1957 and confirmed the decision in 1962. Eventually other countries recognized that thalidomide is extremely teratogenic and is a directly causative amanuensis of phocomelia in neonates. In the late 1950s and early on 1960s, more 10,000 children in 46 countries were born with deformities such as phocomelia as a direct consequence of thalidomide use.29 Thalidomide was first developed past the German Drug Company of Chemie Grünenthal in 1957 under the name of Contergan. It was primarily prescribed every bit a sedative or hypnotic, Chemie Grünenthal besides claimed thalidomide could be used to cure "feet, insomnia, gastritis, and tension"30 and hence its use for Hyperemesis gravidarum – which turned out to be a grave fault.
Thalidomide is still used for a number of atmospheric condition including Erythema Nodosum Leprosum – (an ancient infectious disease caused past Mycobacterium leprae that affects the skin and peripheral nerves), Multiple Myeloma (in combination with dexamethasone), a multifariousness of other cancers, for some symptoms of HIV/AIDS, Sarcoidosis, Crohn's Illness, Graft-versus-Host Affliction, Rheumatoid Arthritis and a number of skin atmospheric condition that take not responded to usual treatment31,32(Effigy 3).
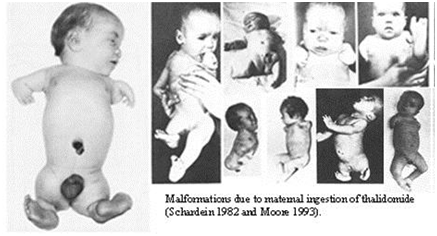
Figure 3 Maleformations due to maternal ingestion of thalidomide (Schardein 1982 and Moore 1992).
Prior to putting ANY female person patient of kid-bearing age on thalidomide for whatsoever of these conditions, the prescribing physician must make certain the patient is non significant and she must exist strongly warned against becoming pregnant while on this drug. Thalidomide is classified by the U.S. Nutrient and Drug Administration (www.fda.com) as a Pregnancy Category X Drug and according to the FDA. "Studies in animals or humans take demonstrated fetal abnormalities and/or there is positive testify of homo fetal risk based on adverse reaction data from investigational or marketing experience, and the risks involved in utilize of the drug in pregnant women conspicuously outweigh potential benefits."
Phocomelia is an extremely rare built skeletal disorder that characteristically affects the limbs and was directly linked to mothers taking thalidomide for morning sickness or hyperemesis gravidarum. It can affect either the upper limbs, lower limbs or both, ordinarily expressing this disorder with severe shortening of upper limb bones. Phocomelia tin also nowadays as astringent, various abnormalities to the face, limbs, ears, nose, vessels and many other underdevelopments. Under no circumstances should a pregnant woman be given thalidomide.
Determination
Hyperemesis gravidarum is from the Greek hyper-, meaning excessive and emesis,meaning airsickness and the Latin gravidarum, the feminine genitive plural grade of an adjective. Here information technology is used as a noun, meaning "pregnant [woman]". Therefore, Hyperemesis gravidarum means "excessive vomiting of pregnant women".
Hyperemesis gravidarum is a serious, life-threatening condition that occurs duringpregnancy. Information technology is treatable, mostly past supportive ways, vitamins, IV Fluids, bland nutrition and family unit support. Do not let a patient with suspected Hyperemesis gravidarum leave your office without developing a treatment plan. Remember these patients tin can "crash" rapidly from stupor, fluid loss, electrolyte imbalance and all the other issues listed in this all-encompassing review of Hyperemesis gravidarum.
A great portion of this document was defended to the differential diagnoses as we practise non want you to miss something, thinking information technology is Hyperemesis gravidarum as many disease processes can mimic Hyperemesis gravidarum. If yous even slightly suspect Hyperemesis gravidarum, treat it and worry nigh your differential investigation at alater time. Patients have been known to endure from Hyperemesis gravidarum for weeks prior to seeking treatment and by the time they get to encounter you in the emergency room, you may have a massive problem on your easily. Be aggressive in your treatment – however it is best to avoid Hyperemesis gravidarum altogether if possible by being proactive when your patient comes in for her first Obstetrical Visit. Give your patient a simplified version of what she needs to watch for, whether it is her first baby or her sixth babe. Never assume the patient knows what to do. Educate your patient (and yourself) to avert whatever futurity complications. Remember, our goal and just goal in Obstetrics is to accept a good for you female parent and infant go dwelling.
Acknowledgements
None.
Disharmonize of interest
The writer declares no conflict of involvement.
References
- Ferri FF. Hyperemesis Gravidarum. Clinical Advisor 2015. 1st ed. Philadelphia, The states; 2004.
- Summers A. Emergency management of hyperemesis gravidarum. Emerg Nurse. 2012;xx(iv):24–28.
- Goodwin TM. Hyperemesis gravidarum. Obstet Gynecol Clin North Am. 2008;35(3):401–417.
- Dodds L, Roughshod DB, Joseph KS, et al. Outcomes of pregnancies complicated by hyperemesis gravidarum. Obstet Gynecol. 2006;107(ii Pt 1):285–292.
- Niebyl JR. Clinical do. Nausea and vomiting in pregnancy. N Engl J Med. 2010;363(16):1544–1550.
- Erick Miriam. Managing Morning Sickness: A Survival Guide for Pregnant Women. United states of america: Grinnen Barrett Publishing; 2004.
- HG Theories & Research helpher.org. Retrieved 25 Dec 2012.
- Cole LA. Biological functions of hCG and hCG-related molecules. Reprod Biol Endocrinol. 2010;8:102.
- Hershman JM. Physiological and pathological aspects of the issue of homo chorionic gonadotropin on the thyroid. Best Pract Res Clin Endocrinol Metab. 2004;eighteen(2):249–265.
- Ahmed KT, Almashhrawi AA, Rahman RN, et al. Liver diseases in pregnancy: diseases unique to pregnancy. World J Gastroenterol. 2013;19(43):7639–7646.
- Matthews DC, Syed AA. The office of TSH receptor antibodies in the management of graves' disease. Eur J Intern Med. 2011;22(3):213–216.
- Carlson Karen J, Eisenstat Stephanie J, et al. The New Harvard Guide to Women's Health. U.s.a.: Harvard Academy Press; 2004. 202 p.
- HER Foundation. Do I take forenoon sickness or HG?. 2012.
- Sheehan P. Hyperemesis gravidarum-assessment and management. Aust Fam Physician. 2007;36(9):698–701.
- Aka N, Atalay S, Sayharman S, et al. Leptin and leptin receptor levels in pregnant women with hyperemesis gravidarum. Aust N Z J Obstet Gynaecol. 2006;46(4):274–277.
- Hyperemesis Gravidarum. (Severe nausea and vomiting during pregnancy). Cleveland Clinic. 2012.
- National institute of health. Hyperemesis gravidarum; 2012.
- Fejzo MS, Poursharif B, MacGibbon RN, et al. Extreme Weight Loss and Extended Duration of Symptoms Common in Hyperemesis Gravidarum. USA: University of Southern California; 2003.
- Björnsdottir S, Cnattingius S, Brandt Fifty, et al. Addison'south affliction in women is a hazard cistron for an adverse pregnancy consequence. J Clin Endocrinol Metab. 2010;95(12):5249–5257.
- Ramin KD. Diabetic ketoacidosis in pregnancy. Obstet Gynecol Clin Northward Am. 1999;26(3):481–488.
- Tuot D, Gibson Southward, Caughey AB, et al. Intradialytic hyperalimentation every bit adjuvant support in pregnant hemodialysis patients: example study and review of the literature. Int Urol Nephrol. 2010;42(1):233–237.
- Jarvis S, Nelson-Piercy C. Management of nausea and vomiting in pregnancy. BMJ. 2011;342:d3606.
- Tan PC, Omar SZ. Contemporary approaches to hyperemesis during pregnancy. Curr Opin Obstet Gynecol. 2011;23(2):87–93.
- Tamay AG, Kuşçu NK. Hyperemesis gravidarum: current aspect. J Obstet Gynaecol. 2011;31(8):708–712.
- Koren K. Motherisk update. Is ondansetron safe for utilise during pregnancy? Can Fam Dr.. 2012;58(10):1092–1093.
- Arthur T Evans. Manual of Obstetrics. 7th ed. Philadelphia, The states; 2007. p. 265–268.
- Bourne Th, Condous 1000. Handbook of Early Pregnancy Care. London, UK: Informa Healthcare; 2006. p. 149–154.
- Matthews A, Haas DM, O Mathúna DP, et al. Interventions for nausea and airsickness in early pregnancy. Cochrane Database Syst Rev. 2010;(9):CD007575.
- Turning points of history-prescription for disaster. History Goggle box Archived from the original; 2011.
- Miller MT. Thalidomide embryopathy: a model for the written report of congenital incomitant horizontal strabismus. Trans Am Ophthalmol Soc. 1991;81:623–674.
- Thalidomide. The American society of health–arrangement pharmacists; 2014.
- British National Formulary (BNF). Drugs Used in Nausea and Vertigo-Vomiting of Pregnancy. 45th ed. UK; 2003.

©2015 Obrowski, et al. This is an open access article distributed nether the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.
Source: https://medcraveonline.com/MOJWH/hyperemesis-gravidarum-a-serious-issue-during-pregnancy-in-depth-clinical-review-and-treatment-modalities.html
0 Response to "Untreated Hyperemesis Can Lead to Preterm Birth. What Is the Cause of the Preterm Birth?"
Post a Comment